Hepatic Artery Embolization
Embolization is a therapy to treat liver tumors by blocking their blood supply. Because liver tumors thrive on highly oxygenated blood from the hepatic artery, blocking that supply may kill it. Embolization is often used to treat tumors not amenable to surgery (liver resection) or as a bridging therapy to "downstage" a tumor to the point a patient is eligible to receive a liver transplant. At a minimum, these procedures can extend life and improve quality of life.
Hepatic Artery Embolization
Using embolization by itself (without delivery of chemotherapy) is known as "bland" hepatic artery embolization, Here, a mixture of contrast (dye) material and small particles is injected into the hepatic artery to stop its blood supply from reaching the tumor. This procedure simply embolizes (blocks and cuts off the blood supply) by mechanical means. The tumor itself is not treated with toxic agents.
Chemoembolization
Chemoembolization, also known as Transarterial Chemoembolization (TACE), adds the delivery of chemotherapeutic agents to the blockade of the tumor. Chemoembolization is used to treat primary liver cancer [hepatocellular carcinoma (HCC)] as well as and liver metastases through the local delivery of cytotoxic chemotherapy to the tumor and blocking of its blood supply.
TACE is a minimally invasive procedure performed by an interventional radiologist. First, cytotoxic chemotherapy is injected via a delivery catheter into the hepatic artery, the feeding blood supply for the tumor. This exposes the tumor to a much higher concentration of chemotherapy, and for a longer time, than would be possible with systemic chemotherapy which is distributed through the entire body. Local delivery of chemo also drastically reduces the toxicity and side effects associated with chemotherapy such as hair loss and nausea.
The second step is to embolize or blocked the hepatic artery by infusing it with occlusive or blocking agents. These are delivered either concurrently with the chemotherapy or subsequent to it through the same delivery catheter. The dual effect is poison the tumor and to cut off the oxygen-rich blood supply from the hepatic artery essential to its growth. The embolization of the tumor also potentiates (increases) the effectiveness of the chemotherapy, creating a synergistic effect between the two.
Key Advantages of Chemoembolization
- Tumor is deprived of oxygen and nutrients.
- Because the drugs are injected directly into the tumor site, the dosage can be 20 to 200 times greater than standard systemic chemotherapy.
- Because the artery is blocked, blood does not wash through the tumor allowing the drugs to persist in the tumor for as long as a month.
- There are fewer side effects because the drugs are trapped in the liver and do not circulate throughout the body
Drug Eluting Beads (DEB TACE)
This is a specific application of TACE which use drug eluting beads. Interventional radiologists inject a solution of chemotherapy-eluting beads into the small branches of the hepatic artery. These beads, about 50 μ in diameter, have been incubated with a chemotherapy agent such as doxorubicin, which releases into the liver over time.
The beads clog the branches of the hepatic artery, cutting off the oxygen supply to the tumors and also deliver a deliver staggered does of targeted chemotherapy over a period of time. Recent studies show that only about 5 percent of the chemotherapy circulates in the bloodstream with DEB-TACE, resulting in fewer side effects than systemic chemotherapy. Similarly, beads containing yttrium-90 that release radiation may be used in a targeted, well-tolerated manner.
 Case Study Slide Show
Case Study Slide Show
Treating Multiple Liver Tumors with Drug Eluting Beads (DEB TACE)
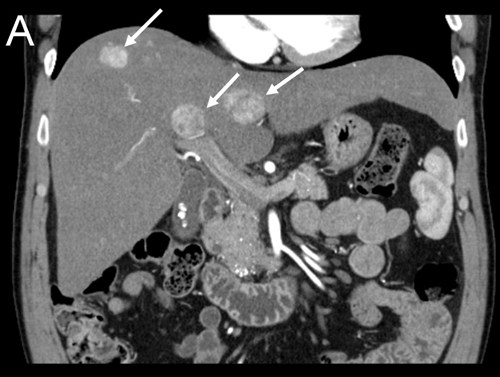 |
| (A) Coronal CT-scan of patient with multiple liver tumors |
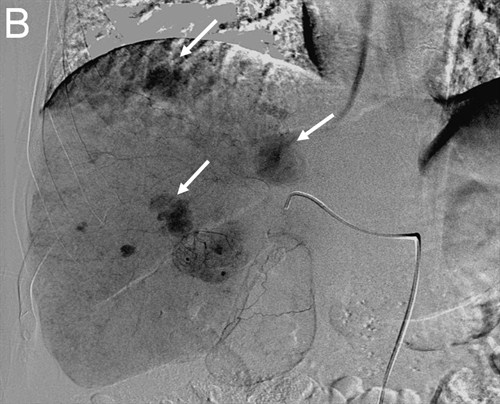 |
| (B) Delayed right liver angiogram showing multiple tumor "blushes" |
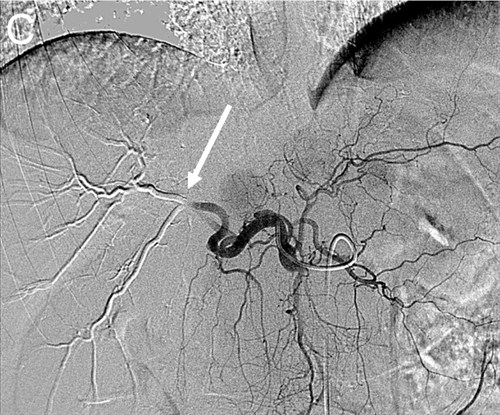 |
| (C) Angiogram after right hepatic artery(white arrow) embolization using Drug Eluting Beads (DEB TACE) |